
Tata Aig Medicare Select
Claim settlement Ratio 95% Network Hospital 10000+
Claim settlement Ratio 95% Network Hospital 10000+
TATA AIG MediCare Select
TATA AIG MediCare Select is TATA AIG’s newly launched comprehensive health insurance plan designed to provide flexible and customizable coverage for individuals and families in India. This modern health insurance policy includes all the essential or basic features such as in-patient hospitalization, pre and post-hospitalization expenses, daycare procedures, and other standard medical benefits. Along with this, it offers unlimited reinstatement of the sum insured, which means if your coverage gets exhausted during the policy year due to a claim, it will be restored for future medical expenses within the same year.
What makes this plan more attractive is its customization option. If you want to enhance your coverage with modern features, you can add optional covers as per your needs. The plan allows you to include OPD benefits for doctor consultations, diagnostics, and pharmacy bills, maternity and new born cover, consumables cover, and wellness-related benefits through add-ons. This flexibility helps you design a health insurance plan that truly matches your lifestyle and medical requirements.
The plan also offers high sum insured options, making it suitable for those who want strong financial protection against rising healthcare costs. There is no entry age limit, which means people of different age groups can opt for this policy. Backed by a trusted brand, TATA AIG has a claim settlement ratio of around 95%, reflecting its reliability and strong customer service support. Moreover, with access to 10,000+ network hospitals across India, policyholders can easily avail cashless treatment in most cities.
Eligibility of TATA AIG Medicare Select Plan
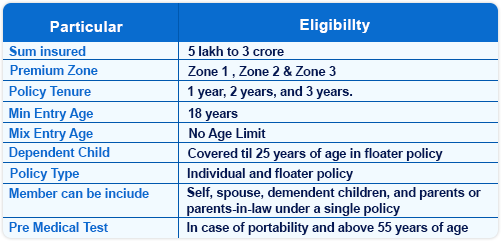
If you are planning to buy Tata Aig MediCare Select Health Insurance, the first step is to understand its eligibility criteria and who can opt for this comprehensive plan. Let’s explore who can purchase this policy, what age groups are generally eligible, and what sum insured and coverage options are available under the plan. Below are the key eligibility highlights of Tata Aig MediCare Select, including entry age, coverage type, and available sum insured options.

Key Features of TATA AIG MediCare Select
TATA AIG MediCare Select is designed with a range of powerful features that aim to provide complete and flexible health insurance coverage for individuals and families. In this section, let’s take a closer look at what key features this plan offers and how they help you strengthen and enhance your overall medical protection. From essential benefits to optional add-ons, this policy is built to adapt to your healthcare needs. Below, we will explore all the important features in detail and understand how they can add real value to your health insurance plan.
1. In-Patient Hospitalisation – Covers room rent, ICU, medicines, doctor fees, surgery, and all admissible medical expenses up to Sum Insured.
2. Room Rent Eligibility – Single Pvt AC room
3. Pre Hospitalisation Expenses – Medical expenses incurred before getting admitted are covered for up to 90 days prior to hospitalization.
4. Post Hospitalisation Expenses – Expenses after discharge are covered for up to 90 days.
5. Day-Care Treatments – All Listed Procedures are covered that require less than 24 hours of hospitalization due to advanced technology. Examples include: Cataract surgery, Chemotherapy, Dialysis, Stone etc.
6. Organ Donor Cover – Covers surgery and medical expenses for the organ donor if you undergo for an organ transplant.
7. Domiciliary Hospitalization – If you need treatment at home because hospital beds are not available or you cannot be moved, the plan covers home hospitalization.
8. AYUSH Treatment – Treatment taken in Ayurveda, Yoga, Unani, Siddha, or Homeopathy is covered.
9. Ambulance Cover – Covers the cost of medically necessary ambulance services in emergencies up to the sum insured.
10. Daily Cash Benefit (Over & above Base Sum Insured) – If you choose a shared room during hospitalization, you get extra cash benefit Twin sharing 1,200 per day and Multi-sharing 1,500 per day.
Restore Infinity Plus – Unlimited reinstatement of the base sum insured if it gets exhausted due to claims.
Cumulative Bonus – Get 50% of Sum Insured every claim-free year, maximum up to 100% OR choose a 1% Discount on Renewal Premium. If a claim is made, the bonus reduces by 50% in the next policy year. You can avail either the Cumulative Bonus or the Renewal Premium Discount not both.
Add Ons of TATA AIG MediCare Select
Enhance your Tata AIG MediCare Select plan with these powerful add-on riders designed to increase coverage, reduce out-of-pocket expenses, and provide specialized health benefits:
1. Consumable Benefit Rider – This rider covers the cost of specified non-payable items listed under Annexure I, used during hospitalization.
2. Supercharge Bonus Rider – Get 100% of sum insured guaranteed bonus on every year maximum up to 500%, even if you make claims.
3. Infinite Advantage Rider – This rider removes any limit on the base sum insured for one approved claim during the lifetime of the policy. Works for both Inpatient Treatment and Day Care Procedures. Offers financial protection against exceptionally large medical bills.
4. Home Care Treatment Rider – Covers expenses for treatments taken at home, up to the Sum Insured. Helps patients who require medical care but not hospitalization. Pandemic Care coverage included up to 25% of the Sum Insured. Ensures comfort and convenience while still offering quality care.
5. Accidental Death Benefit Rider – If the insured suffers an accident that leads to death within 365 days, Tata AIG pays 100% of the Sum Insured, or 50, 00,000, whichever is lower. This rider provides financial security to the family in case of accidental death.
6. Preventive Annual Health Check-up Rider – Covers a cashless preventive health check-up once every policy year through Tata AIG’s authorized service providers. Ensures regular monitoring of health and early detection of medical conditions.
7. Cancer Benefit Rider – Provides a lump-sum pay-out if the insured person is diagnosed with Cancer of Specified Severity during the policy period. This amount can be used for Treatment costs, Second opinions, Lifestyle adjustments, financial support during recovery
8. Women Suraksha Rider – Specially designed for female insured members. Includes three components:
a. She Care+ – Covers specific consultations arranged through the insurer’s empanelled providers.
b. Polycystic Ovarian Disease/Syndrome Cover – Covers diagnostic evaluation and treatment prescribed for PCOD/PCOS and irregular menstrual cycles.
c. Women+ Screening & Vaccination – Includes cancer screening tests and cervical cancer vaccination, promoting preventive health for women.
9. Emergency Air Ambulance Rider – Covers cost of emergency air ambulance services for life-threatening conditions that require urgent transfer to another hospital for better medical management.
10. Health Condition Management Program – Provides specialized health management support, including, Consultations, Condition monitoring, customized improvement programs. Ideal for individuals with lifestyle diseases needing controlled health management.
11. Advanced Cover Rider – Reduces the waiting period for select pre-existing diseases from standard periods to just 30 days for, Type 2 Diabetes, Hypertension, Hyperlipidaemia, and Asthma. A valuable rider for those with lifestyle-related health conditions.
12. Domestic Second Opinion Rider – Provides a second medical opinion from certified medical experts within India for listed critical illnesses. Helps ensure correct diagnosis and treatment decisions.
13. International Second Opinion Rider – Offers access to global medical experts outside India for a second opinion on listed serious illnesses. Useful for rare or complex conditions.
14. Mental Wellbeing Rider Package – This plan also offers a complete mental health support system, recognizing the importance of emotional and psychological well-being along with physical health. It includes annual mental health screening through empanelled providers, helping in early identification and timely support for mental health concerns. The policy further covers professional psychological therapy sessions and counselling for mental and behavioural issues, ensuring access to expert care when needed. It also includes diet consultations with certified nutritionists or dieticians to promote better physical and mental wellness.
In addition, the plan provides vocational rehabilitation support for individuals whose mental health conditions affect their ability to work, along with access to stress management and mental wellness programs. An addiction cessation program is also available, offering professional support to help individuals overcome substance dependency in a structured and supportive manner.
15. Additional Sum Insured for Accidental Hospitalization – Provides extra Sum Insured exclusively for hospitalization resulting from accidental injuries. Helps handle sudden medical emergencies without exhausting the base policy coverage.
16. Pocket Saver 2.0 Rider (OPD Rider) – This plan offers a comprehensive outpatient (OPD) benefit designed to cover everyday medical needs beyond hospitalization. It includes OPD consultations and diagnostic tests for illnesses or injuries (non-preventive), ensuring that routine doctor visits and necessary investigations are financially supported. In addition, the policy also provides coverage for OPD dental care, including consultations and specified treatments as per the policy terms. Vision care benefits are included as well, covering ophthalmologist consultations and corrective lenses once every two policy years. To make healthcare more accessible, the plan also offers unlimited tele-consultations through empaneled medical professionals. Overall, this OPD benefit is ideal for families who require frequent doctor visits and want complete outpatient coverage under their health insurance plan.
17. Maternity Care Rider – This plan covers complete maternity-related expenses after a waiting period of 2 years, ensuring financial support during one of the most important phases of life. It includes coverage for both normal and C-section deliveries, along with any pregnancy-related complications that may arise. In addition, the policy also takes care of newborn baby expenses, including medical care and first-year vaccinations. Overall, it offers comprehensive support during pregnancy and early motherhood, helping families manage medical costs with greater peace of mind.
18. Reduction of Maternity Waiting Period – Reduces the maternity waiting period to just 1 year of continuous coverage, making maternity benefits accessible sooner.
Discounts Available of TATA AIG MediCare Select
TATA AIG MediCare Select also offers attractive discount opportunities that can help reduce your overall health insurance premium. While the exact discount structure may vary, policyholders can benefit from savings based on factors like policy tenure, family coverage selection, and healthy lifestyle choices. These discount options are designed to make comprehensive health insurance more affordable without compromising on coverage. In the section below, let’s explore what types of premium discounts may be available under the TATA AIG MediCare Select plan and how they can help you optimize your policy cost:
a. Young Family Discount – 10% (all insured ≤40 years)
b. Professional Discount – 7.5% (salaried professionals)
c. Long Term Discount – 5% (2 yrs), 7.5% (3 yrs)
d. Family Floater Discount – Up to 32%
e. Multi-Individual Discount – 5%
f. Favourable Experience Discount – Up to 20%
Waiting Periods of TATA AIG MediCare Select
When buying TATA AIG MediCare Select Health Insurance, it is also important to understand the waiting period applicable under the plan. Like most comprehensive health insurance policies in India, certain illnesses, pre-existing diseases, and specific treatments may have a defined waiting period before you can make a claim for them.
Typically, there is an initial waiting period from the policy start date, along with separate waiting periods for pre-existing medical conditions and specified illnesses. However, some benefits may be covered after shorter durations or even from day one, depending on the coverage selected and add-ons chosen.
Understanding the waiting period helps you plan your coverage better and avoid surprises at the time of claim. Below, we will look at the different types of waiting periods applicable under the TATA AIG MediCare Select plan in detail.
a. 30 days initial waiting period
b. 24 months for specified diseases
c. 36 months for Pre-existing diseases (PED)
d. 24 months for Maternity Expenses (Reduce to 1 year by opting Rider)
Exclusions of TATA AIG MediCare Select
Before purchasing TATA AIG MediCare Select Health Insurance, it is equally important to understand the exclusions under the plan. Exclusions are specific medical conditions, treatments, or situations that are not covered by the policy, either permanently or for a certain period. Like most comprehensive health insurance plans in India, this policy may not cover expenses arising from non-medical treatments, cosmetic or aesthetic procedures (unless medically necessary), self-inflicted injuries, or treatments not backed by medical advice. Certain conditions may also be excluded during the waiting period.
Being aware of the exclusions helps you make an informed decision and avoid confusion at the time of claim. In the section below, we will review the key exclusions of the TATA AIG MediCare Select plan in detail so you clearly understand what is not covered under this health insurance policy.
a. Investigation & Evaluation
b. Rest Cure, rehabilitation and respite care
c. Obesity/Weight Control
d. Change-of-gender treatments
e. Cosmetic or plastic Surgery
f. Hazardous or Adventure sports
g. Breach of law
h. Treatment for Alcoholism, drug or substance abuse or any addictive condition and consequences thereof.
i. Refractive Error
j.Unproven Treatments
k.Sterility and Infertility
Claim Process of TATA AIG MediCare Select
Understanding the claim process of TATA AIG MediCare Select Health Insurance is important to ensure a smooth and hassle-free experience during medical emergencies. The insurer offers both cashless and reimbursement claim options, giving policyholders flexibility based on the hospital and situation.
For cashless treatment, you can visit any of the 10,000+ network hospitals associated with TATA AIG and inform the hospital’s insurance desk about your policy details. After submitting the required documents and pre-authorization form, the insurer reviews the request and directly settles the approved medical bills with the hospital.
In case you choose treatment at a non-network hospital, you can opt for a reimbursement claim by paying the bills upfront and later submitting all original documents, discharge summaries, and claim forms to TATA AIG for settlement. Once verified, the approved claim amount is reimbursed to your registered bank account. With a strong claim settlement ratio of around 95%, TATA AIG aims to provide reliable and efficient claim support to its policyholders, ensuring financial peace of mind during medical emergencies.
1. Cashless Claim - You need to intimate the TPA at least 48 hours before a planned admission, and in case of an emergency, within 24 hours of hospitalization. Once you reach the hospital, submit all the required documents at the insurance TPA desk for verification. After the documents are reviewed and approval is received, you can proceed with your cashless treatment without any upfront payment hassles.
2. Reimbursement Claim - After discharge, make sure to collect all the required documents, including the discharge summary, hospital invoices, medical reports, a copy of your ID proof, and a cancelled cheque. Once you have all the documents ready, submit them to your insurance company for claim processing. After successful verification, the claim is usually processed within 7–14 working days, and the approved amount is credited to your bank account.
Eligibility of TATA AIG Medicare Select Plan
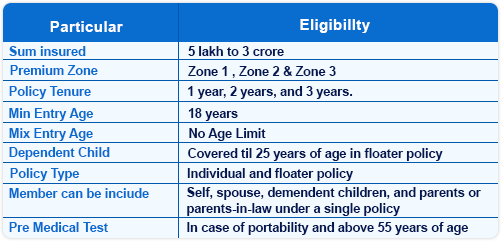
If you are planning to buy Tata Aig MediCare Select Health Insurance, the first step is to understand its eligibility criteria and who can opt for this comprehensive plan. Let’s explore who can purchase this policy, what age groups are generally eligible, and what sum insured and coverage options are available under the plan. Below are the key eligibility highlights of Tata Aig MediCare Select, including entry age, coverage type, and available sum insured options.
|
Particular |
Eligibility |
|
Sum insured |
5 lakh to 3 crore |
|
Premium Zone |
Zone 1, Zone 2 & Zone 3 |
|
Policy Tenure |
1 year, 2 years, and 3 years. |
|
Min Entry Age |
18 Years |
|
Max Entry Age |
No Age Limit |
|
Dependent Child |
Covered till 25 years of age in floater policy |
|
Policy Type |
Individual and floater policy |
|
Member can be include |
Self, spouse, dependent children, and parents or parents-in-law under a single policy |
|
Pre Medical Test |
In case of portability and above 55 years of age |
Key Features of TATA AIG MediCare Select
TATA AIG MediCare Select is designed with a range of powerful features that aim to provide complete and flexible health insurance coverage for individuals and families. In this section, let’s take a closer look at what key features this plan offers and how they help you strengthen and enhance your overall medical protection. From essential benefits to optional add-ons, this policy is built to adapt to your healthcare needs. Below, we will explore all the important features in detail and understand how they can add real value to your health insurance plan.
1. In-Patient Hospitalisation – Covers room rent, ICU, medicines, doctor fees, surgery, and all admissible medical expenses up to Sum Insured.
2. Room Rent Eligibility – Single Pvt AC room
3. Pre Hospitalisation Expenses – Medical expenses incurred before getting admitted are covered for up to 90 days prior to hospitalization.
4. Post Hospitalisation Expenses – Expenses after discharge are covered for up to 90 days.
5. Day-Care Treatments – All Listed Procedures are covered that require less than 24 hours of hospitalization due to advanced technology. Examples include: Cataract surgery, Chemotherapy, Dialysis, Stone etc.
6. Organ Donor Cover – Covers surgery and medical expenses for the organ donor if you undergo for an organ transplant.
7. Domiciliary Hospitalization – If you need treatment at home because hospital beds are not available or you cannot be moved, the plan covers home hospitalization.
8. AYUSH Treatment – Treatment taken in Ayurveda, Yoga, Unani, Siddha, or Homeopathy is covered.
9. Ambulance Cover – Covers the cost of medically necessary ambulance services in emergencies up to the sum insured.
10. Daily Cash Benefit (Over & above Base Sum Insured) – If you choose a shared room during hospitalization, you get extra cash benefit Twin sharing 1,200 per day and Multi-sharing 1,500 per day.
Restore Infinity Plus – Unlimited reinstatement of the base sum insured if it gets exhausted due to claims.
Cumulative Bonus – Get 50% of Sum Insured every claim-free year, maximum up to 100% OR choose a 1% Discount on Renewal Premium. If a claim is made, the bonus reduces by 50% in the next policy year. You can avail either the Cumulative Bonus or the Renewal Premium Discount not both.
Add Ons of TATA AIG MediCare Select
Enhance your Tata AIG MediCare Select plan with these powerful add-on riders designed to increase coverage, reduce out-of-pocket expenses, and provide specialized health benefits:
1. Consumable Benefit Rider – This rider covers the cost of specified non-payable items listed under Annexure I, used during hospitalization.
2. Supercharge Bonus Rider – Get 100% of sum insured guaranteed bonus on every year maximum up to 500%, even if you make claims.
3. Infinite Advantage Rider – This rider removes any limit on the base sum insured for one approved claim during the lifetime of the policy. Works for both Inpatient Treatment and Day Care Procedures. Offers financial protection against exceptionally large medical bills.
4. Home Care Treatment Rider – Covers expenses for treatments taken at home, up to the Sum Insured. Helps patients who require medical care but not hospitalization. Pandemic Care coverage included up to 25% of the Sum Insured. Ensures comfort and convenience while still offering quality care.
5. Accidental Death Benefit Rider – If the insured suffers an accident that leads to death within 365 days, Tata AIG pays 100% of the Sum Insured, or 50, 00,000, whichever is lower. This rider provides financial security to the family in case of accidental death.
6. Preventive Annual Health Check-up Rider – Covers a cashless preventive health check-up once every policy year through Tata AIG’s authorized service providers. Ensures regular monitoring of health and early detection of medical conditions.
7. Cancer Benefit Rider – Provides a lump-sum pay-out if the insured person is diagnosed with Cancer of Specified Severity during the policy period. This amount can be used for Treatment costs, Second opinions, Lifestyle adjustments, financial support during recovery
8. Women Suraksha Rider – Specially designed for female insured members. Includes three components:
a. She Care+ – Covers specific consultations arranged through the insurer’s empanelled providers.
b. Polycystic Ovarian Disease/Syndrome Cover – Covers diagnostic evaluation and treatment prescribed for PCOD/PCOS and irregular menstrual cycles.
c. Women+ Screening & Vaccination – Includes cancer screening tests and cervical cancer vaccination, promoting preventive health for women.
9. Emergency Air Ambulance Rider – Covers cost of emergency air ambulance services for life-threatening conditions that require urgent transfer to another hospital for better medical management.
10. Health Condition Management Program – Provides specialized health management support, including, Consultations, Condition monitoring, customized improvement programs. Ideal for individuals with lifestyle diseases needing controlled health management.
11. Advanced Cover Rider – Reduces the waiting period for select pre-existing diseases from standard periods to just 30 days for, Type 2 Diabetes, Hypertension, Hyperlipidaemia, and Asthma. A valuable rider for those with lifestyle-related health conditions.
12. Domestic Second Opinion Rider – Provides a second medical opinion from certified medical experts within India for listed critical illnesses. Helps ensure correct diagnosis and treatment decisions.
13. International Second Opinion Rider – Offers access to global medical experts outside India for a second opinion on listed serious illnesses. Useful for rare or complex conditions.
14. Mental Wellbeing Rider Package – This plan also offers a complete mental health support system, recognizing the importance of emotional and psychological well-being along with physical health. It includes annual mental health screening through empanelled providers, helping in early identification and timely support for mental health concerns. The policy further covers professional psychological therapy sessions and counselling for mental and behavioural issues, ensuring access to expert care when needed. It also includes diet consultations with certified nutritionists or dieticians to promote better physical and mental wellness.
In addition, the plan provides vocational rehabilitation support for individuals whose mental health conditions affect their ability to work, along with access to stress management and mental wellness programs. An addiction cessation program is also available, offering professional support to help individuals overcome substance dependency in a structured and supportive manner.
15. Additional Sum Insured for Accidental Hospitalization – Provides extra Sum Insured exclusively for hospitalization resulting from accidental injuries. Helps handle sudden medical emergencies without exhausting the base policy coverage.
16. Pocket Saver 2.0 Rider (OPD Rider) – This plan offers a comprehensive outpatient (OPD) benefit designed to cover everyday medical needs beyond hospitalization. It includes OPD consultations and diagnostic tests for illnesses or injuries (non-preventive), ensuring that routine doctor visits and necessary investigations are financially supported. In addition, the policy also provides coverage for OPD dental care, including consultations and specified treatments as per the policy terms. Vision care benefits are included as well, covering ophthalmologist consultations and corrective lenses once every two policy years. To make healthcare more accessible, the plan also offers unlimited tele-consultations through empaneled medical professionals. Overall, this OPD benefit is ideal for families who require frequent doctor visits and want complete outpatient coverage under their health insurance plan.
17. Maternity Care Rider – This plan covers complete maternity-related expenses after a waiting period of 2 years, ensuring financial support during one of the most important phases of life. It includes coverage for both normal and C-section deliveries, along with any pregnancy-related complications that may arise. In addition, the policy also takes care of newborn baby expenses, including medical care and first-year vaccinations. Overall, it offers comprehensive support during pregnancy and early motherhood, helping families manage medical costs with greater peace of mind.
18. Reduction of Maternity Waiting Period – Reduces the maternity waiting period to just 1 year of continuous coverage, making maternity benefits accessible sooner.
Discounts Available of TATA AIG MediCare Select
TATA AIG MediCare Select also offers attractive discount opportunities that can help reduce your overall health insurance premium. While the exact discount structure may vary, policyholders can benefit from savings based on factors like policy tenure, family coverage selection, and healthy lifestyle choices. These discount options are designed to make comprehensive health insurance more affordable without compromising on coverage. In the section below, let’s explore what types of premium discounts may be available under the TATA AIG MediCare Select plan and how they can help you optimize your policy cost:
a. Young Family Discount – 10% (all insured ≤40 years)
b. Professional Discount – 7.5% (salaried professionals)
c. Long Term Discount – 5% (2 yrs), 7.5% (3 yrs)
d. Family Floater Discount – Up to 32%
e. Multi-Individual Discount – 5%
f. Favourable Experience Discount – Up to 20%
Waiting Periods of TATA AIG MediCare Select
When buying TATA AIG MediCare Select Health Insurance, it is also important to understand the waiting period applicable under the plan. Like most comprehensive health insurance policies in India, certain illnesses, pre-existing diseases, and specific treatments may have a defined waiting period before you can make a claim for them.
Typically, there is an initial waiting period from the policy start date, along with separate waiting periods for pre-existing medical conditions and specified illnesses. However, some benefits may be covered after shorter durations or even from day one, depending on the coverage selected and add-ons chosen.
Understanding the waiting period helps you plan your coverage better and avoid surprises at the time of claim. Below, we will look at the different types of waiting periods applicable under the TATA AIG MediCare Select plan in detail.
a. 30 days initial waiting period
b. 24 months for specified diseases
c. 36 months for Pre-existing diseases (PED)
d. 24 months for Maternity Expenses (Reduce to 1 year by opting Rider)
Exclusions of TATA AIG MediCare Select
Before purchasing TATA AIG MediCare Select Health Insurance, it is equally important to understand the exclusions under the plan. Exclusions are specific medical conditions, treatments, or situations that are not covered by the policy, either permanently or for a certain period. Like most comprehensive health insurance plans in India, this policy may not cover expenses arising from non-medical treatments, cosmetic or aesthetic procedures (unless medically necessary), self-inflicted injuries, or treatments not backed by medical advice. Certain conditions may also be excluded during the waiting period.
Being aware of the exclusions helps you make an informed decision and avoid confusion at the time of claim. In the section below, we will review the key exclusions of the TATA AIG MediCare Select plan in detail so you clearly understand what is not covered under this health insurance policy.
a. Investigation & Evaluation
b. Rest Cure, rehabilitation and respite care
c. Obesity/Weight Control
d. Change-of-gender treatments
e. Cosmetic or plastic Surgery
f. Hazardous or Adventure sports
g. Breach of law
h. Treatment for Alcoholism, drug or substance abuse or any addictive condition and consequences thereof.
i. Refractive Error
j.Unproven Treatments
k.Sterility and Infertility
Claim Process of TATA AIG MediCare Select
Understanding the claim process of TATA AIG MediCare Select Health Insurance is important to ensure a smooth and hassle-free experience during medical emergencies. The insurer offers both cashless and reimbursement claim options, giving policyholders flexibility based on the hospital and situation.
For cashless treatment, you can visit any of the 10,000+ network hospitals associated with TATA AIG and inform the hospital’s insurance desk about your policy details. After submitting the required documents and pre-authorization form, the insurer reviews the request and directly settles the approved medical bills with the hospital.
In case you choose treatment at a non-network hospital, you can opt for a reimbursement claim by paying the bills upfront and later submitting all original documents, discharge summaries, and claim forms to TATA AIG for settlement. Once verified, the approved claim amount is reimbursed to your registered bank account. With a strong claim settlement ratio of around 95%, TATA AIG aims to provide reliable and efficient claim support to its policyholders, ensuring financial peace of mind during medical emergencies.
1. Cashless Claim - You need to intimate the TPA at least 48 hours before a planned admission, and in case of an emergency, within 24 hours of hospitalization. Once you reach the hospital, submit all the required documents at the insurance TPA desk for verification. After the documents are reviewed and approval is received, you can proceed with your cashless treatment without any upfront payment hassles.
2. Reimbursement Claim - After discharge, make sure to collect all the required documents, including the discharge summary, hospital invoices, medical reports, a copy of your ID proof, and a cancelled cheque. Once you have all the documents ready, submit them to your insurance company for claim processing. After successful verification, the claim is usually processed within 7–14 working days, and the approved amount is credited to your bank account.


